The Medxoom Difference
Employers, Brokers and Third Party Administrators prefer our health benefits platform because we understand that making decisions for one’s health isn’t just an administrative function; it’s a personal experience. That’s why we spent years carefully developing a best-in-class system that not just saves our clients' time, stress and money – it supports every step towards better health benefits usage and engagement.
Healthcare is too expensive
Total health spending for a family of four with employer coverage tops $22,000+ on average
-
Family Out-of-Pocket Spending
-
Family Premium Contribution
-
Employer Premium Contribution
What makes our healthcare platform different?

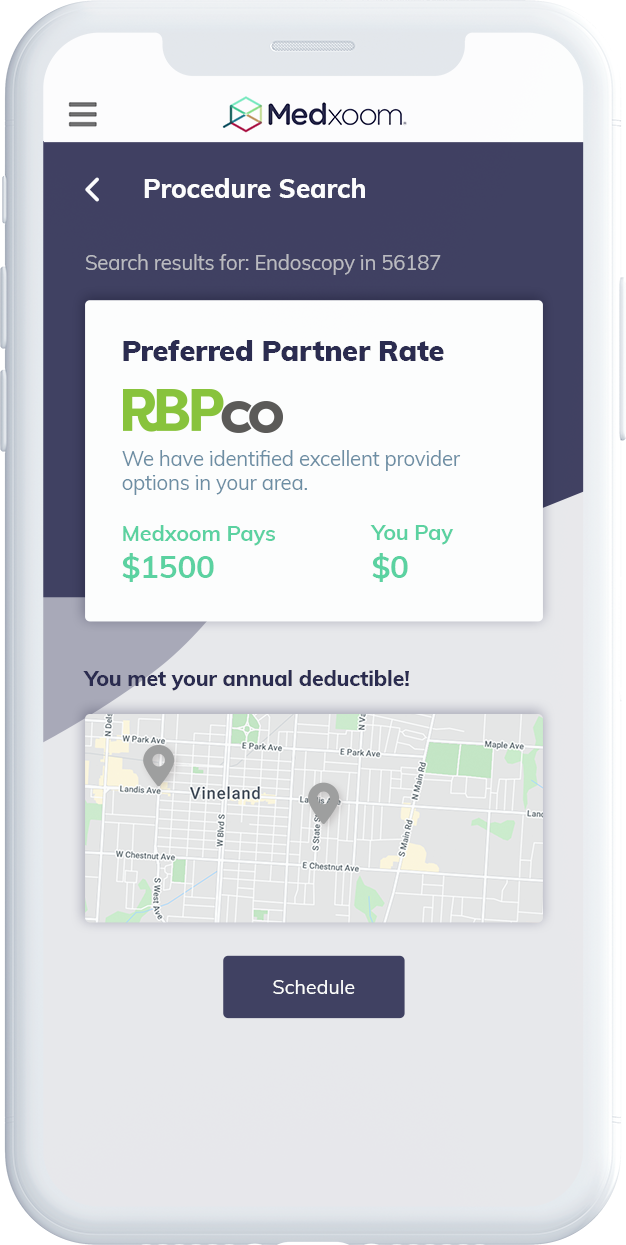
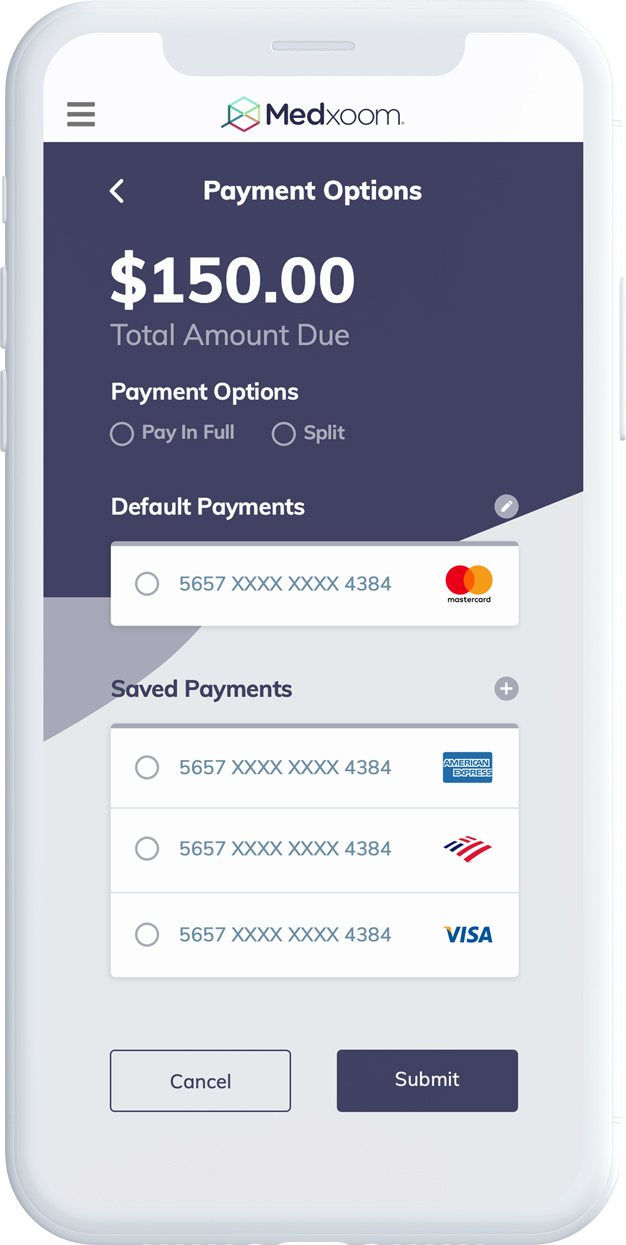
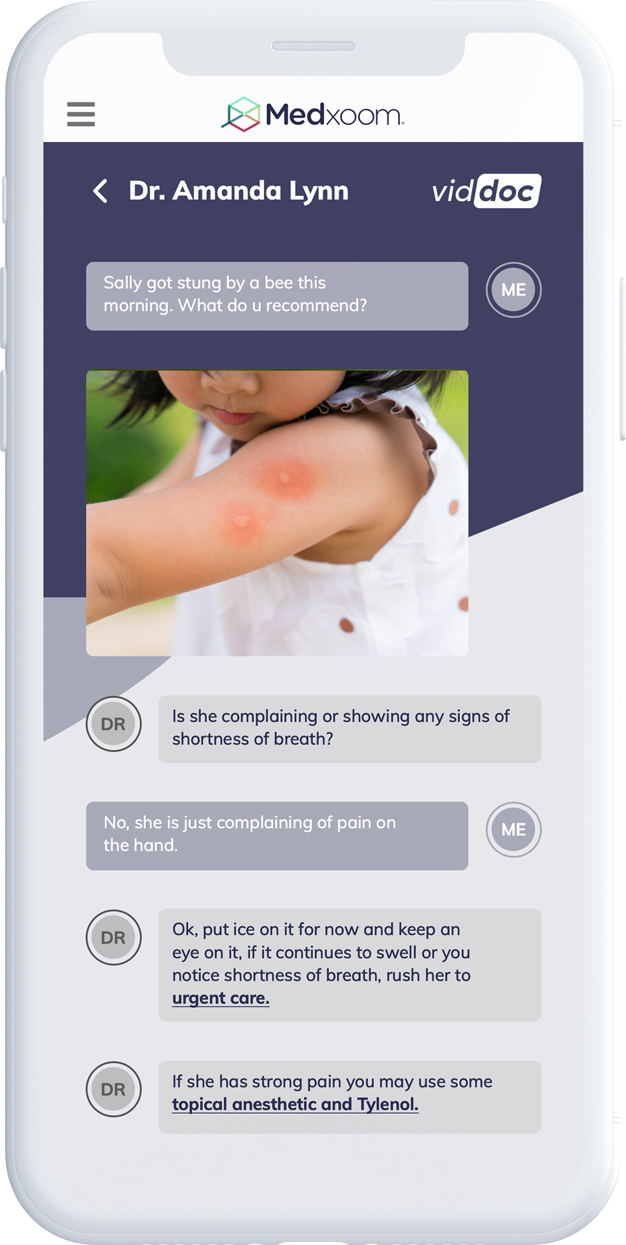
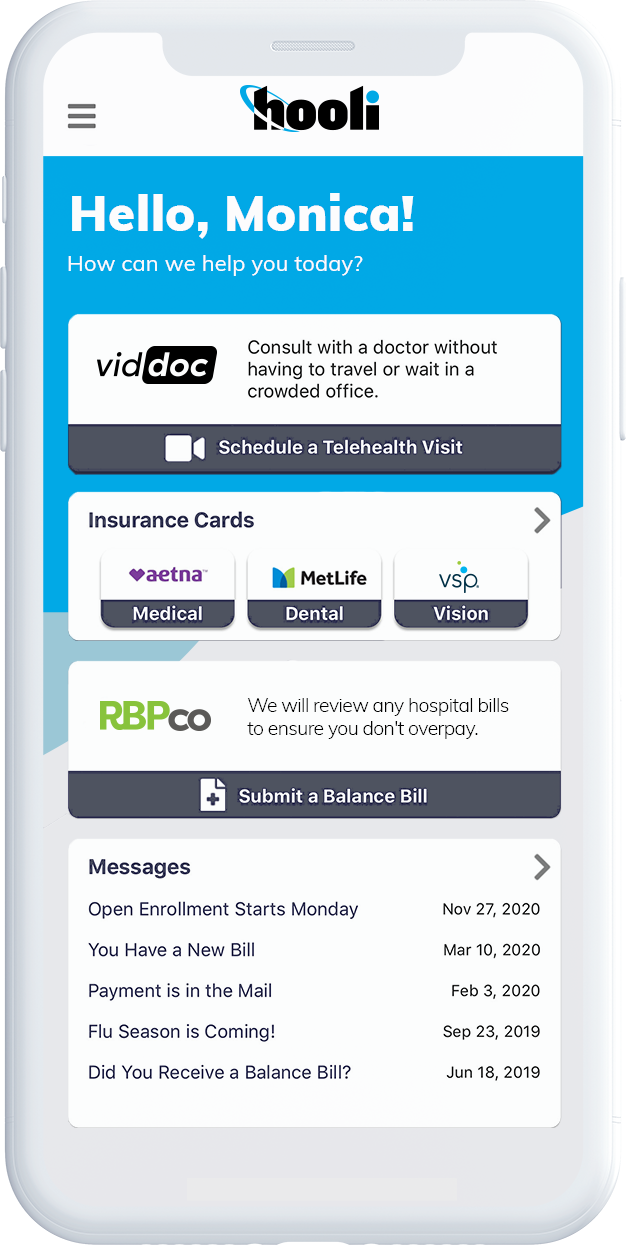
Q&A with Medxoom: Why a Unifying Experience for Health Plan Members is the Only Way to Bring True Value
Featuring Jeff Toewe
Our co-founder and CEO, Jeff Toewe, and our Enterprise Sales Executive, Matt Smith, were guests on The Granite List Live podcast to discuss why cookie-cutter groups don’t create enough value for health plan members.They talk about how they want to understand what their clients are trying to do, the solutions they're trying to utilize to improve that member experience, and drive down that healthcare spend
